How Smart Technology is making a difference in patient’s lives
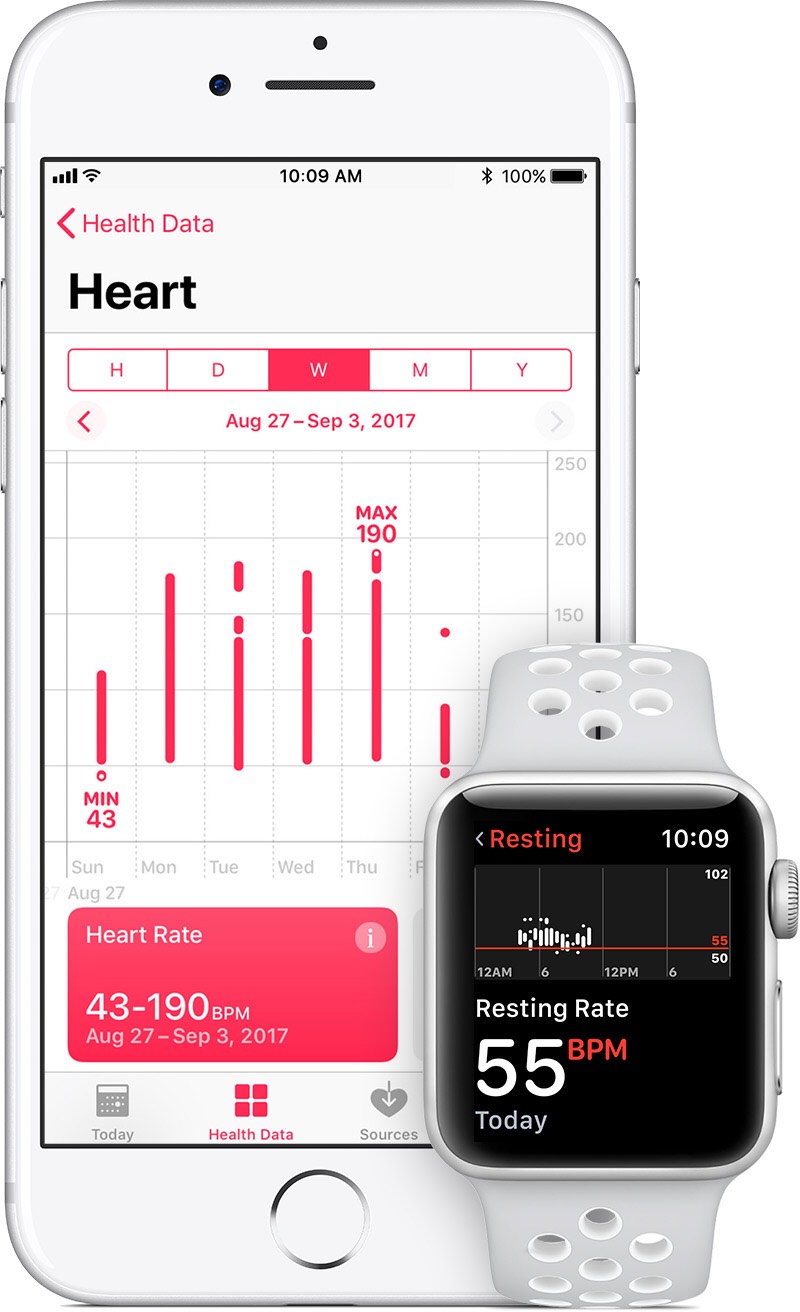 Smart technology in cellphones, tablets and computers have not only revolutionized our daily lives but how we also monitor our health. More specifically, the Apple Watch, one of the most popular smart wristwatches in the world, has become a great tool for patients to monitor their heart health. Recently, there have been stories of patients discovering irregularities in their heart rate because of notifications from their smart watch. Apple has teamed up with Stanford Medicine to form the “Apple Heart Study”, which uses data from the Apple Watch to identify irregular heart rhythms, as well as potentially serious heart conditions. Apple then uses the information gathered to improve its technology which is designed to detect and analyze irregular heart rhythms. If irregularities are discovered with a person’s heart rate, they then have the option to consult with a telehealth Heart Study Cardiologist. The Cardiologist then may do further observations of the patient while wearing a small “e-patch”, which will gather important data and give a clearer picture of the perceived issues, as well as give recommendations to the patient’s primary health care provider. What does this mean for most patients? Millions of Americans experience the common form of hearth arrhythmia known Atrial Fibrillation or “A-fib”. For most people, it is undiagnosed, and can often come and go regularly, especially if set off by certain stimulants such as alcohol, caffeine and other substances. Although a person may see their primary care physician with regularity, heart arrhythmias may not show up on the EKG, unless they are experiencing “A-Fib” at that exact moment. In addition, these undetected arrhythmias are among the leading causes of stroke. The more monitoring that a patient has, the better chance that irregularities are caught at an earlier stage before a stroke occurs. Therefore, heart monitoring devices such as the Apple Watch, may be beneficial to senior patients, as well as those who are more susceptible to heart attacks and arrhythmias. As is the case with most technology, there is definitely room for improvement. It is possible that the watch may pick up on arrhythmias if a person enjoys their morning coffee or has an intense workout session at the gym. However, the overall benefit is positively overwhelming. Most people may stigmatize that heart health only affects seniors or morbidly obese individuals, but this is far from the case. Recently, a teenager received an alert from her smart watch that her heart rate was unusually high. Besides a headache and a small bout of shortness of breath, she reportedly felt normal. Once she received another alert from her watch, she went to the emergency room. Doctors then identified that she was suffering from chronic kidney disease, and if it were not for the alerts from her watch, it is very possible that the disease may have continued to go undetected and potentially have devastating effects. The benefits of the smart watch are not only good for seniors or those looking to lose weight, it is effective for all, no matter their age, gender or physical ailments.
Smart technology in cellphones, tablets and computers have not only revolutionized our daily lives but how we also monitor our health. More specifically, the Apple Watch, one of the most popular smart wristwatches in the world, has become a great tool for patients to monitor their heart health. Recently, there have been stories of patients discovering irregularities in their heart rate because of notifications from their smart watch. Apple has teamed up with Stanford Medicine to form the “Apple Heart Study”, which uses data from the Apple Watch to identify irregular heart rhythms, as well as potentially serious heart conditions. Apple then uses the information gathered to improve its technology which is designed to detect and analyze irregular heart rhythms. If irregularities are discovered with a person’s heart rate, they then have the option to consult with a telehealth Heart Study Cardiologist. The Cardiologist then may do further observations of the patient while wearing a small “e-patch”, which will gather important data and give a clearer picture of the perceived issues, as well as give recommendations to the patient’s primary health care provider. What does this mean for most patients? Millions of Americans experience the common form of hearth arrhythmia known Atrial Fibrillation or “A-fib”. For most people, it is undiagnosed, and can often come and go regularly, especially if set off by certain stimulants such as alcohol, caffeine and other substances. Although a person may see their primary care physician with regularity, heart arrhythmias may not show up on the EKG, unless they are experiencing “A-Fib” at that exact moment. In addition, these undetected arrhythmias are among the leading causes of stroke. The more monitoring that a patient has, the better chance that irregularities are caught at an earlier stage before a stroke occurs. Therefore, heart monitoring devices such as the Apple Watch, may be beneficial to senior patients, as well as those who are more susceptible to heart attacks and arrhythmias. As is the case with most technology, there is definitely room for improvement. It is possible that the watch may pick up on arrhythmias if a person enjoys their morning coffee or has an intense workout session at the gym. However, the overall benefit is positively overwhelming. Most people may stigmatize that heart health only affects seniors or morbidly obese individuals, but this is far from the case. Recently, a teenager received an alert from her smart watch that her heart rate was unusually high. Besides a headache and a small bout of shortness of breath, she reportedly felt normal. Once she received another alert from her watch, she went to the emergency room. Doctors then identified that she was suffering from chronic kidney disease, and if it were not for the alerts from her watch, it is very possible that the disease may have continued to go undetected and potentially have devastating effects. The benefits of the smart watch are not only good for seniors or those looking to lose weight, it is effective for all, no matter their age, gender or physical ailments.






 hat is almost never talked about. In most of these neighborhoods, depression was seen as a “white issue” and being bipolar meant that you were just crazy. Having suicidal thoughts meant that you were weak-minded. Growing up, I was taught that the sole treatment for most mental issues was going to church and relying solely on prayer. The stigma of mental health was like that faded stain in your favorite shirt; no matter how much you try to scrub it and clean it, it still shows up. 1 in 5 Americans will experience a mental health issue, yet most will not seek treatment. According to the National Alliance of Mental Illness (NAMI), the leading mental health advocacy organization in the country, African Americans and Hispanic Americans only seek treatment at half the rate of their White counterparts. However due to the recent alarming increase of mass shootings and celebrities making controversial, shocking statements, mental health is now in the consciousness of most Americans, and more specifically the black community. The key is treating mental health just as one treats diabetes, hypertension or any other chronic condition. Mental wellness is a large, complicated issue and it may require treatment from mental health professionals (i.e. therapists, psychiatrists) who can help diagnose symptoms and develop successful treatment plans similar to a person with heart issues going to visit a cardiologist or having a cavity and going to visit the dentist. Normalizing the idea of mental health treatment through education not only helps the affected person, it teaches society how to treat them as well. Social acceptance, general encouragement and support from friends and family may help keep people on the right track as well. Making mental health normal is not only necessary, it’s the first step in erasing the myth that you have to be a certain skin color or belong in a selective tax bracket to be affected. In addition, most people who are struggling with mental illness feel alone. They feel isolated and disconnected from society. It is a huge burden for a person to carry and can only lead them further down the rabbit hole. These individuals should be encouraged to share their experiences with others who are going through the same illnesses. During my senior year in high school, my 3-year-old nephew was shot and killed in an accident and as a result, I struggled with depression for several months. Blaming myself for his loss. I hardly slept and could barely eat. It felt like I was sleepwalking through life, trapped in a constant fog of sadness, helplessness and anger. Why did it happen? Why didn’t I do more? I had questions that I felt no one could answer. It was only after talking with others who experienced the pain and heartache of loss, as well as going to therapy with an open heart and mind, that I was able to recover and release. Confronting my emotions and doubts instead of burying them. I had to reteach my brain that accepting help is ok and that we are all vulnerable sometimes, and that sometimes your greatest strength comes from being weak. I had to unlearn lessons which my community taught me; That as a black man, you keep everything inside and show no emotions. Our community must learn that talking about mental health is not a “white thing”, or a “rich people” or a “woman” thing, it needs to be for everyone, regardless of where you come from or the color of your skin; and this is the first step that we can take to not only break the stigma, but permanently delete the stereotype.
hat is almost never talked about. In most of these neighborhoods, depression was seen as a “white issue” and being bipolar meant that you were just crazy. Having suicidal thoughts meant that you were weak-minded. Growing up, I was taught that the sole treatment for most mental issues was going to church and relying solely on prayer. The stigma of mental health was like that faded stain in your favorite shirt; no matter how much you try to scrub it and clean it, it still shows up. 1 in 5 Americans will experience a mental health issue, yet most will not seek treatment. According to the National Alliance of Mental Illness (NAMI), the leading mental health advocacy organization in the country, African Americans and Hispanic Americans only seek treatment at half the rate of their White counterparts. However due to the recent alarming increase of mass shootings and celebrities making controversial, shocking statements, mental health is now in the consciousness of most Americans, and more specifically the black community. The key is treating mental health just as one treats diabetes, hypertension or any other chronic condition. Mental wellness is a large, complicated issue and it may require treatment from mental health professionals (i.e. therapists, psychiatrists) who can help diagnose symptoms and develop successful treatment plans similar to a person with heart issues going to visit a cardiologist or having a cavity and going to visit the dentist. Normalizing the idea of mental health treatment through education not only helps the affected person, it teaches society how to treat them as well. Social acceptance, general encouragement and support from friends and family may help keep people on the right track as well. Making mental health normal is not only necessary, it’s the first step in erasing the myth that you have to be a certain skin color or belong in a selective tax bracket to be affected. In addition, most people who are struggling with mental illness feel alone. They feel isolated and disconnected from society. It is a huge burden for a person to carry and can only lead them further down the rabbit hole. These individuals should be encouraged to share their experiences with others who are going through the same illnesses. During my senior year in high school, my 3-year-old nephew was shot and killed in an accident and as a result, I struggled with depression for several months. Blaming myself for his loss. I hardly slept and could barely eat. It felt like I was sleepwalking through life, trapped in a constant fog of sadness, helplessness and anger. Why did it happen? Why didn’t I do more? I had questions that I felt no one could answer. It was only after talking with others who experienced the pain and heartache of loss, as well as going to therapy with an open heart and mind, that I was able to recover and release. Confronting my emotions and doubts instead of burying them. I had to reteach my brain that accepting help is ok and that we are all vulnerable sometimes, and that sometimes your greatest strength comes from being weak. I had to unlearn lessons which my community taught me; That as a black man, you keep everything inside and show no emotions. Our community must learn that talking about mental health is not a “white thing”, or a “rich people” or a “woman” thing, it needs to be for everyone, regardless of where you come from or the color of your skin; and this is the first step that we can take to not only break the stigma, but permanently delete the stereotype.